Emergency Response

Emergency Response in the OMXUS system is a decentralized, proximity-based mutual aid network that replaces centralized emergency dispatch with direct community mobilization. When a member activates an alert — by tapping their NFC ring — every nearby OMXUS participant receives an immediate notification via mesh network, and the nearest available people respond physically. The system is designed to achieve a median first-responder contact time of under 60 seconds in areas with sufficient network density, compared to the 7–14 minute average of professional emergency medical services in urban areas and 14–30 minutes in rural settings.[1]
The term "emergency response" is deliberately chosen and deliberately redefined. In conventional usage, it refers to the deployment of professional, state-funded services — police, fire, ambulance — following a reported emergency. OMXUS redefines it as the immediate mobilization of proximate community members as the primary response layer, with professional services as a secondary escalation. This redefinition rests on a specific thesis: the most critical variable in emergency outcomes is not the skill of the responder but the speed of first contact, and the fastest possible contact comes from people who are already nearby, not from professionals dispatched from a distance.
Background and Rationale
The Response Time Problem
Emergency medicine research has established a well-documented relationship between response time and outcomes across multiple emergency types. The relationship is not linear — it follows a curve of rapidly diminishing survivability:
| Emergency Type | Critical Window | Survival Rate (Within Window) | Survival Rate (Beyond Window) | Source |
|---|---|---|---|---|
| Cardiac arrest | 4–6 minutes | 40–50% with bystander CPR | <10% without intervention | AHA 2020[2] |
| Choking/airway obstruction | 4–10 minutes | >90% with intervention | Rapidly fatal | ERC 2021[3] |
| Severe hemorrhage | 5–15 minutes | High with direct pressure | ~33% mortality if uncontrolled | Eastridge et al. (2012)[4] |
| Anaphylaxis | 5–30 minutes | >95% with epinephrine | Fatal in ~1% of cases | Simons et al. (2011)[5] |
| Violent assault (ongoing) | Seconds to minutes | Intervention interrupts harm | Harm continues until cessation | — |
| Stroke | 3–4.5 hours (thrombolytics) | Significantly improved outcomes | Permanent disability risk | Powers et al. (2019)[6] |
The critical insight is that for the most time-sensitive emergencies — cardiac arrest, choking, hemorrhage, physical violence — the window is measured in minutes, and frequently in fewer minutes than any centralized dispatch system can deliver a professional responder. This is not a failure of professional services; it is a structural limitation of the dispatch model, which requires sequential steps (call → assess → dispatch → travel → arrive) that each consume time regardless of how efficiently they are executed.
Why Existing Systems Cannot Close the Gap

The modern emergency dispatch model, established in the late 20th century (the 9-1-1 system was introduced in the United States in 1968, and Australia's Triple Zero (000) has operated since 1961), was a transformative improvement over previous arrangements. However, the architecture has inherent latency that cannot be optimized away:
- Call processing — The caller must communicate with a dispatcher, describe the situation, and provide a location. Studies show this takes a median of 60–90 seconds even with trained dispatchers.[7]
- Dispatch decision — The dispatcher must determine which unit to send. This adds 30–60 seconds.
- Travel time — The dispatched unit must physically travel to the location. The NFPA standard (NFPA 1710) targets 4 minutes of travel time for first-arriving engine companies, but compliance varies widely.[1]
- On-scene setup — The responder must locate the patient, assess the scene, and begin intervention.
The total chain, even in well-funded urban systems, produces a median response time of 7–14 minutes.[8] In rural, remote, or under-resourced areas, response times of 20–45 minutes are common. In many nations, ambulance services do not exist at all for large portions of the population.
This is not a problem that can be solved by hiring more paramedics or building more stations. The latency is architectural. OMXUS proposes a different architecture.
The Proximity Thesis
The OMXUS emergency response model rests on a specific, testable thesis:
This thesis draws on three bodies of research:
1. Bystander intervention research. The bystander effect, first documented by social psychologists John Darley and Bibb Latané following the 1964 murder of Kitty Genovese, established that the probability of any individual helping in an emergency decreases as the number of bystanders increases — a phenomenon called diffusion of responsibility.[9] However, subsequent research has identified clear moderating factors: bystanders are far more likely to intervene when (a) they receive a direct, personal alert, (b) they perceive clear responsibility to act, and (c) they have minimal ambiguity about the situation.[10] OMXUS emergency alerts are designed to activate all three moderating factors: the alert is personal (directed to your device), clear (someone near you needs help), and assigns responsibility (you are one of the nearest people).
2. Collective efficacy research. Sociologist Robert Sampson's research on collective efficacy — the combination of mutual trust and willingness to intervene for the common good — demonstrated that neighborhoods with high collective efficacy experience dramatically lower rates of violence, independent of socioeconomic composition.[11] OMXUS emergency response is, in effect, collective efficacy as infrastructure — a system that makes the willingness to intervene easy to express and the mutual trust verifiable through the web of trust.
3. Community first responder programs. Empirical evidence from existing community responder programs supports the proximity thesis. The GoodSAM app in the United Kingdom alerts nearby CPR-trained volunteers when a cardiac arrest is detected, achieving median alert-to-arrival times of under 6 minutes — nearly halving the traditional ambulance response time.[12] The PulsePoint app in the United States has shown similar results. These programs demonstrate the principle at small scale; OMXUS generalizes it to a universal, always-on network.
The 60-Second Target
Derivation
The 60-second target for median first-responder contact is not arbitrary. It is derived from a calculation involving three variables:
- Network density — The number of OMXUS participants per unit area
- Alert propagation time — The time for an emergency alert to reach nearby devices
- Physical travel time — The time for the nearest alerted person to reach the location
For urban areas with a network density of ≥500 participants per square kilometer (equivalent to roughly 1 in 20 adults in a city like Sydney or Melbourne):
- Average distance to nearest participant: ~45 meters (derived from spatial Poisson distribution)
- Alert propagation time: <5 seconds via mesh network (device-to-device, no internet dependency)
- Walking/running time for 45 meters: ~20–40 seconds at brisk walk to jog
This yields a total of approximately 25–45 seconds from activation to first contact, well within the 60-second target.
At lower densities (rural areas, early adoption phases), the 60-second target is not achievable. The system acknowledges this explicitly — the target is conditional on density, not a universal promise. In low-density environments, the system still provides value by reducing response time relative to centralized dispatch, even if the absolute time is measured in minutes rather than seconds.
| Network Density (per km²) | Avg. Distance to Nearest | Estimated Alert-to-Contact | Comparison with 000/EMS |
|---|---|---|---|
| 2,000+ (dense urban) | ~22m | 15–30 seconds | 7–14 min (EMS) |
| 500–2,000 (urban) | ~45m | 25–45 seconds | 7–14 min (EMS) |
| 100–500 (suburban) | ~100m | 1–3 minutes | 10–20 min (EMS) |
| 10–100 (rural) | ~300m | 3–10 minutes | 20–45 min (EMS) |
| <10 (remote) | >1km | 10+ minutes | 30–60+ min or unavailable |
What "60 Seconds" Means and Does Not Mean
The 60-second figure refers to:
- Median first-contact time, not a guarantee
- First contact by any community member, not arrival of professional medical care
- Achievable at sufficient network density (≥500/km²), not universally
- Physical presence of a person, not necessarily a trained medical responder
It does not replace professional emergency services. It supplements them by providing immediate human presence during the critical minutes before professionals arrive. The community responder can:
- Begin CPR or apply a defibrillator
- Apply direct pressure to bleeding
- Place a person in the recovery position
- Provide safety through witness presence
- Call professional services with accurate, real-time information
- Comfort and reassure
How the System Works
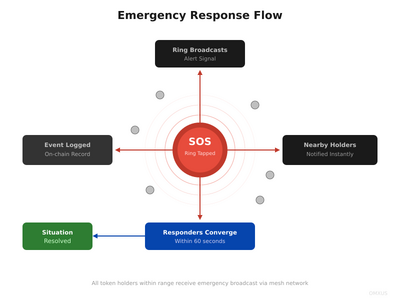
The system operates through three phases: activation, propagation, and response. Each phase is designed to minimize latency while maximizing reliability across different infrastructure conditions.
Activation
Emergency activation uses the NFC ring with a deliberate gesture pattern (double-tap or sustained hold) designed to prevent accidental activation while remaining accessible under stress. The gesture was chosen based on research into motor function under acute stress, which shows that fine motor skills degrade while gross motor actions remain intact.[13]
Upon activation:
- The ring broadcasts an emergency signal via Bluetooth Low Energy to the member's paired device
- The device constructs an emergency packet containing: location (GPS + mesh-derived), member identity (cryptographic), timestamp, and emergency type (if specified)
- The packet propagates through the mesh network — phone-to-phone via Wi-Fi Direct, Yggdrasil overlay, and LoRa radio fallback
- Every OMXUS device within range receives the alert within seconds
Alert Propagation

The alert travels through multiple redundant channels simultaneously, ensuring delivery even under infrastructure failure:
| Channel | Range | Latency | Dependency | Failure Mode |
|---|---|---|---|---|
| BLE direct | ~100m | <1 second | None (device-to-device) | Receiver must be in range |
| Wi-Fi Direct mesh | ~200m per hop | 1–3 seconds | None (device-to-device) | Limited indoor penetration |
| Yggdrasil overlay | City-wide | 2–5 seconds | Internet connectivity | Fails without internet |
| LoRa radio | 2–15km | 5–15 seconds | LoRa hardware | Requires LoRa-equipped devices |
| Meshtastic relay | 1–5km per hop | 5–30 seconds | Meshtastic nodes | Depends on node placement |
The multi-channel design means the system degrades gracefully: if internet is down, mesh and LoRa still function. If cell towers fail, device-to-device communication continues. This resilience is particularly important because emergencies often coincide with infrastructure failures (natural disasters, power outages, civil unrest).
Response Protocol
When a community member receives an alert:
- Acknowledge — Tap to confirm availability. This is broadcast back, so the person in need knows help is coming, and other responders can coordinate rather than duplicate.
- Move toward — Head to the indicated location. The device provides direction and distance.
- Assess — Upon arrival, determine what help is needed.
- Assist — Provide appropriate aid (first aid, safety presence, comfort).
- Escalate — If professional help is needed, call emergency services with accurate, first-hand information about the situation.
- Stay — Remain until the situation is resolved or professional responders arrive.
Privacy Architecture
Location data is handled according to the Telemetry for Humans principle:
- No continuous tracking — The system does not monitor member locations. There is no location history, no movement database, no geofencing.
- Emergency-only broadcast — Location is shared only upon activation, only to nearby devices, and only for the duration of the emergency.
- Cryptographic identity — The alert includes the member's verified identity (so responders know who they are helping and that the alert is genuine), but this identity is anchored to the web of trust, not to a government database.
- No post-hoc surveillance — Emergency response data is not retained for later analysis by authorities. The data serves the emergency and then ceases to exist in identifiable form.
The Deeper Purpose
Redefining Emergency Response
The conventional concept of "emergency response" places responsibility for community safety in the hands of a professional class — police, firefighters, paramedics — funded by the state and dispatched from centralized facilities. Citizens are positioned as callers: their role in an emergency is to observe, report, and wait.
OMXUS redefines emergency response as a community function in which every member is both a potential caller and a potential responder. This is not voluntarism in the conventional sense (unpaid labour substituting for funded services). It is a structural redefinition of where the primary responsibility for immediate safety resides: not in institutions, but in the relationships between proximate people.
This redefinition draws on the OMXUS principle of Justice as Prevention: the most effective way to prevent harm is to ensure that no person is ever isolated from the community around them. Emergency response, in this framing, is not primarily about reacting to emergencies. It is about structurally eliminating the conditions that allow emergencies to escalate.
Universal Witness and Crime Prevention
The emergency response network creates what OMXUS terms universal witness — the condition in which any person, at any time, can make their situation visible to the surrounding community with a single gesture. This has a direct bearing on crime prevention:
Much violent and predatory crime depends on the isolation of the victim from witnesses and potential interveners. The criminological concept of routine activity theory, developed by Cohen and Felson (1979), holds that crime requires the convergence of three elements: a motivated offender, a suitable target, and the absence of capable guardians.[14]
OMXUS emergency response directly addresses the third element. By enabling any person to summon capable guardians — nearby community members who have agreed to respond — within seconds, the system eliminates the isolation that predatory behaviour requires. The effect is not merely reactive (responding to crime in progress) but preventive: the knowledge that any potential victim can instantly summon multiple witnesses and responders changes the cost-benefit calculation for potential offenders.
This is consistent with Sampson's finding that perceived collective efficacy — the belief that neighbors would intervene — is as predictive of low crime rates as actual intervention.[11] The system's value is partly in what it does (mobilize responders) and partly in what it represents (the certainty that mobilization will occur).
Eliminating the Bystander Effect
The bystander effect is one of the most robust findings in social psychology: in group settings, individuals are less likely to help because responsibility is diffused across all observers. The OMXUS alert system is designed to counteract the three psychological mechanisms that produce the bystander effect:
| Mechanism | Description | How OMXUS Counteracts It |
|---|---|---|
| Diffusion of responsibility | "Someone else will help" | Alert assigns personal responsibility; acknowledgment system shows who is responding |
| Pluralistic ignorance | "Others aren't reacting, so it must not be serious" | Alert is explicit: this is an emergency, help is requested |
| Evaluation apprehension | Fear of embarrassment if the situation isn't really an emergency | Cryptographic verification confirms the alert is genuine; social norm of response is established |
Research by Fischer et al. (2011) demonstrated that the bystander effect is significantly reduced when the emergency is clearly dangerous (rather than ambiguous) and when the cost of intervention is low.[15] OMXUS emergency alerts are designed to satisfy both conditions: the alert communicates clear danger, and the response (move toward, be present) has low personal cost.
Historical Context
Evolution of Emergency Response Systems
The concept of organized emergency response has evolved through several phases:
| Era | Model | Response Agent | Typical Response Time |
|---|---|---|---|
| Pre-modern | Community self-help | Neighbors, family | Variable (immediate to hours) |
| 19th century | Organized fire brigades, early police | Professional responders | 10–30 minutes |
| Mid-20th century | Centralized dispatch (000, 911, 999) | Professional responders via dispatch | 7–20 minutes |
| Late 20th century | Enhanced dispatch (GPS, CAD systems) | Professional responders with better routing | 5–15 minutes |
| Early 21st century | Community first responder apps (GoodSAM, PulsePoint) | Trained volunteers + professionals | 3–6 minutes (volunteers) + professional EMS |
| OMXUS model | Universal community network | Every proximate member + professional escalation | <60 seconds (proximate members) + professional EMS |
The trajectory shows a pattern: each innovation has reduced response time by bringing the responder closer to the emergency. OMXUS represents the logical endpoint of this trajectory — the responder is not dispatched at all, but is already there.
Precedents in Community Emergency Response
Several existing programs demonstrate elements of the OMXUS model:
- CERT (USA) — FEMA-sponsored teams of trained community volunteers who respond to disasters. Demonstrates that non-professionals can provide effective emergency response. Limitation: requires formal training and organizational structure.
- GoodSAM (UK/Global) — Mobile app alerting nearby CPR-trained individuals to cardiac arrests. Achieves faster response than ambulance alone. Limitation: single emergency type, requires opt-in training registration.
- Hatzalah (Global) — Volunteer EMS organizations in Jewish communities, achieving some of the fastest ambulance response times in the world (often under 3 minutes in dense areas). Demonstrates that community-embedded responders outperform centralized dispatch. Limitation: community-specific, requires trained volunteers.
- Neighborhood watch programs — Demonstrate willingness of community members to participate in collective safety, though typically focused on reporting rather than direct response.
OMXUS differs from all of these in scope (every member, not trained volunteers), activation method (ring tap, not phone call), communication layer (mesh network, not cellular/internet), and integration (embedded in a complete governance system, not a standalone service).
Response Obligation and Social Contract
Membership in OMXUS includes an expectation — social, not legal — that members will respond to nearby emergency alerts when they are able. This expectation is part of the mutual aid compact that defines OMXUS participation:
- Not legally mandatory — The system does not and cannot compel physical response. There is no penalty for non-response.
- Socially expected — The cultural norm is that nearby members respond. This norm is reinforced by the web of trust, which is built on relationships of mutual accountability.
- Response is visible — Acknowledgment of alerts is recorded (for coordination, not punishment). Consistent non-response may affect a member's standing within their trust network, but there is no automated penalty.
- Capacity-aware — The system recognizes that not everyone can respond at all times. Physical limitation, personal emergency, distance, and other factors are all legitimate reasons not to respond.
This social contract model is consistent with the OMXUS principle that the system cannot affect individual freedom — it cannot force you to respond. But it creates an environment in which response is easy, expected, and socially valued. The goal is a culture of mutual aid, not a system of compulsion.
Scenarios
Medical Emergency
Sarah, 62, collapses while walking in a park. Her ring detects the sudden change in orientation (accelerometer) and, after a brief confirmation window, broadcasts an emergency alert.
- T+0s: Alert propagates via BLE and Wi-Fi Direct to devices within 200m
- T+5s: Three OMXUS members within 150m receive the alert on their phones
- T+8s: Two members acknowledge — a 28-year-old jogger and a 45-year-old parent at a nearby playground
- T+25s: The jogger reaches Sarah, finds her unconscious, begins assessment
- T+35s: The parent arrives, calls 000, provides exact location and description
- T+45s: Jogger begins CPR (trained through community program)
- T+9min: Ambulance arrives. CPR has been in progress for over 8 minutes.
Without the OMXUS network, Sarah would have been lying alone until a passerby noticed — potentially 5–15 minutes. With cardiac arrest, the difference between CPR at 45 seconds and CPR at 10 minutes is often the difference between life and death. The American Heart Association estimates that bystander CPR doubles or triples survival rates.[2]
Personal Safety
James, 19, is walking home at night and notices he is being followed. He taps his ring.
- T+0s: Alert broadcasts to nearby devices
- T+3s: Six members within 300m receive the alert
- T+10s: Four acknowledge
- T+20s: Two members emerge from nearby houses, moving toward James's location
- T+30s: The person following James sees others approaching and changes direction
- T+45s: James is accompanied by two community members until he reaches home
The situation resolved without confrontation. The mechanism is deterrence through presence — the knowledge that a person can instantly summon witnesses changes the calculus for anyone considering predatory behaviour. This is Sampson's collective efficacy made instantaneous and technological.
Natural Disaster
An earthquake damages infrastructure in a suburban area. Cell towers are down. Internet is offline.
- T+0s: Multiple members activate emergency alerts
- Alerts propagate via LoRa radio and device-to-device mesh — no internet required
- Nearby members receive alerts and begin checking on neighbors
- Community self-organizes into search and response groups
- When professional responders arrive (hours later in disaster scenarios), they find an organized community with accurate information about where help is needed
This scenario illustrates why the mesh network architecture is not a technical curiosity but a safety requirement. Emergencies frequently coincide with the failure of the infrastructure that conventional emergency systems depend on.
Limitations and Honest Assessment
The OMXUS emergency response model has significant limitations that must be acknowledged:
- Density dependency — The 60-second target requires ≥500 participants per km². Below this, response times increase. In sparsely populated areas or during early adoption, the system may not provide faster response than calling 000.
- Training gap — Community responders are not paramedics. They can provide basic first aid and presence, but not advanced medical care. The system supplements professional services, not replaces them.
- False activation — Any system that enables one-tap alerting risks false or accidental activations. Gesture design and confirmation windows mitigate this, but cannot eliminate it.
- Responder safety — Community members responding to emergencies may encounter dangerous situations (violent incidents, hazardous materials, structural collapse). The system must communicate risk clearly and never require responders to enter dangerous situations.
- Adoption threshold — The system provides minimal value until a critical mass of participants exists in a geographic area. This creates a chicken-and-egg problem for adoption.
- Legal liability — Jurisdictions vary in their Good Samaritan protections for community responders. Legal frameworks may need to evolve alongside the system. The Companion Acts address this through proposed legislative changes.
- Equity concerns — If OMXUS adoption correlates with socioeconomic status, the communities most in need of rapid emergency response (low-income, high-crime areas) may have the lowest network density.
These limitations are not reasons to abandon the model, but they are reasons to be honest about what it can and cannot do, and to design adoption strategies that address them directly.
See Also
- Justice as Prevention — The foundational principle that emergency response embodies
- Principles — The six non-negotiable OMXUS principles, including non-maleficence and prevention
- Mesh Networks — The communication infrastructure enabling decentralized alerts
- NFC Technology — The ring hardware used for emergency activation
- Web of Trust — The identity and trust system underlying responder verification
- Crime Prevention Research — Research on structural crime prevention through community cohesion
- Addiction and Connection — Why human connection is the root of community resilience
- Telemetry for Humans — The privacy framework governing emergency location data
- Companion Acts — Proposed legislation including Good Samaritan protections
- Technical Architecture — The four-layer system architecture
- Getting Started — How to join and participate in the OMXUS network
- Main Page
External Links
- Emergency service — Wikipedia overview of conventional emergency services
- Bystander effect — The social psychology phenomenon OMXUS is designed to counteract
- Collective efficacy — Sampson's research on community capacity for self-regulation
- Community Emergency Response Team (CERT) — FEMA's community responder program
- GoodSAM — Existing app-based community cardiac arrest response
- Routine activity theory — Criminological framework relevant to universal witness
- Mutual aid — The organizational principle underlying OMXUS emergency response
References
- ↑ 1.0 1.1 National Fire Protection Association. (2023). Response Time Standards: NFPA 1710 and 1720. NFPA.
- ↑ 2.0 2.1 American Heart Association. (2020). "Heart Disease and Stroke Statistics—2020 Update." Circulation, 141(9), e139–e596.
- ↑ European Resuscitation Council. (2021). ERC Guidelines 2021. Resuscitation, 161, 1–60.
- ↑ Eastridge, B. J., et al. (2012). "Death on the battlefield (2001–2011): Implications for the future of combat casualty care." Journal of Trauma and Acute Care Surgery, 73(6), S431–S437.
- ↑ Simons, F. E. R., et al. (2011). "World Allergy Organization Guidelines for the Assessment and Management of Anaphylaxis." World Allergy Organization Journal, 4(2), 13–37.
- ↑ Powers, W. J., et al. (2019). "Guidelines for the Early Management of Patients With Acute Ischemic Stroke." Stroke, 50(12), e344–e418.
- ↑ Ornato, J. P., et al. (2012). "Impact of improved 911 efficiency on out-of-hospital cardiac arrest survival." Prehospital Emergency Care, 16(2), 196–203.
- ↑ Blackwell, T. H., & Kaufman, J. S. (2002). "Response time effectiveness: Comparison of response time and survival in an urban emergency medical services system." Academic Emergency Medicine, 9(4), 288–295.
- ↑ Darley, J. M., & Latané, B. (1968). "Bystander intervention in emergencies: Diffusion of responsibility." Journal of Personality and Social Psychology, 8(4), 377–383.
- ↑ Fischer, P., et al. (2011). "The bystander-effect: A meta-analytic review on bystander intervention in dangerous and non-dangerous emergencies." Psychological Bulletin, 137(4), 517–537.
- ↑ 11.0 11.1 Sampson, R. J., Raudenbush, S. W., & Earls, F. (1997). "Neighborhoods and Violent Crime: A Multilevel Study of Collective Efficacy." Science, 277(5328), 918–924.
- ↑ Smith, C. M., et al. (2020). "The Use of Community First Responders in Real Emergencies in England." Resuscitation, 155, 152–159.
- ↑ Grossman, D., & Christensen, L. W. (2008). On Combat: The Psychology and Physiology of Deadly Conflict in War and in Peace. Warrior Science Publications.
- ↑ Cohen, L. E., & Felson, M. (1979). "Social Change and Crime Rate Trends: A Routine Activity Approach." American Sociological Review, 44(4), 588–608.
- ↑ Fischer, P., et al. (2011). "The bystander-effect: A meta-analytic review on bystander intervention in dangerous and non-dangerous emergencies." Psychological Bulletin, 137(4), 517–537.
- American Heart Association. (2020). "Heart Disease and Stroke Statistics—2020 Update." Circulation, 141(9), e139–e596.
- Blackwell, T. H., & Kaufman, J. S. (2002). "Response time effectiveness." Academic Emergency Medicine, 9(4), 288–295.
- Cohen, L. E., & Felson, M. (1979). "Social Change and Crime Rate Trends: A Routine Activity Approach." American Sociological Review, 44(4), 588–608.
- Darley, J. M., & Latané, B. (1968). "Bystander intervention in emergencies." Journal of Personality and Social Psychology, 8(4), 377–383.
- Eastridge, B. J., et al. (2012). "Death on the battlefield." Journal of Trauma and Acute Care Surgery, 73(6), S431–S437.
- Fischer, P., et al. (2011). "The bystander-effect: A meta-analytic review." Psychological Bulletin, 137(4), 517–537.
- Grossman, D., & Christensen, L. W. (2008). On Combat. Warrior Science Publications.
- Sampson, R. J., Raudenbush, S. W., & Earls, F. (1997). "Neighborhoods and Violent Crime." Science, 277(5328), 918–924.
- Smith, C. M., et al. (2020). "Community First Responders in Real Emergencies." Resuscitation, 155, 152–159.
Civic Proximity Response System

A civic proximity response system (also called a citizen proximity alert network or distributed emergency response) is a proposed or deployed model of emergency management in which people who are physically near an incident—neighbors, passers-by, trained volunteers, venue staff, or other opt-in "community responders"—are rapidly notified and coordinated alongside formal emergency medical services (EMS), police and fire service dispatch. The concept treats time-to-first-help as a primary determinant of outcomes, and tries to shorten it by making "help is nearby" operational rather than aspirational.
Unlike traditional emergency response, which relies mainly on a centralized dispatcher and professional responders traveling from stations or hospitals, a civic proximity response system assumes that many emergencies occur within reach of other citizens and that a portion of those citizens can safely contribute immediate actions: calling emergency services, providing first aid, performing cardiopulmonary resuscitation (CPR), retrieving an automated external defibrillator (AED), acting as a witness, escorting a person to safety, or de-escalating until authorities arrive. In near-future designs, such systems are often imagined as being initiated by a wearable "help token" (e.g., an NFC ring or bracelet) that can trigger a graded alert with minimal friction.
Background

Emergency response outcomes are strongly influenced by delay. In many time-critical scenarios—such as out-of-hospital cardiac arrest—the probability of survival declines rapidly without early intervention, which motivates systems that increase bystander CPR and early defibrillation. This has led to the growth of community first responder programs and smartphone dispatch of volunteer responders in multiple countries. A 2022 randomized clinical trial evaluated smartphone-aided dispatch of lay volunteers to retrieve AEDs and respond to cardiac arrests, reflecting the broader movement toward technology-mediated bystander mobilization.[1]
The concept also draws on social psychology research on the bystander effect, in which individuals are less likely to intervene when other people are present, often due to diffusion of responsibility and uncertainty about what is happening. Civic proximity response systems aim to counteract these dynamics by converting ambiguous social situations into explicit requests for assistance with clear roles and instructions.
Legal and Ethical Frameworks
Duty to Rescue and "Failure to Assist"
Legal approaches to bystander responsibility vary. Many jurisdictions have some form of Good Samaritan law, primarily offering liability protections for those who provide reasonable aid. A smaller set of jurisdictions impose a duty to rescue or a duty to call for help in defined circumstances.
In France, the offence commonly referred to as non-assistance à personne en danger ("failure to assist a person in danger") is associated with Article 223-6 of the French Penal Code and is explained in official French public guidance as an offence that can carry criminal penalties when someone fails to provide assistance or to obtain assistance without risk to themselves or others.[2] This framework is often cited in discussions of civic response as an attempt to formalize a moral norm: that summoning help is a basic social obligation.
Ethics of Mutual Obligation
Civic proximity response systems are sometimes justified using ideas from civic republicanism, care ethics, and social contract theory: if people benefit from living in a community with shared infrastructure and protections, they may also hold minimal reciprocal duties in emergencies. Critics argue that moral duties should not necessarily be enforceable duties, and that coercive "duty to assist" models can create risk for vulnerable bystanders or lead to misinterpretation in complex incidents.
Technology and System Design
A civic proximity response system may combine several technical components:
- Low-friction initiation: A rapid trigger mechanism such as a smartphone app, wearable button, or NFC ring/bracelet that can be activated under stress. An NFC-based device can, in principle, use "tap to alert" interactions with any compatible reader (e.g., a phone or fixed terminal), reducing the need to unlock a device or navigate menus.
- Location and geofencing: The system uses geolocation (GPS, Wi-Fi, Bluetooth, or cell triangulation) to identify nearby responders and resources (e.g., AEDs, staffed venues, security desks).
- Graded alerting: Alerts may be categorized (medical emergency, personal safety, witness request, welfare check) and may include options for silent escalation.
- Responder tiers and verification: Some designs differentiate between trained responders (e.g., off-duty clinicians), general volunteers, and designated venue staff. Verification may include identity checks, certifications, or background screening.
- Integration with formal dispatch: The system can be connected to emergency call centers so that alerts generate official incidents and share relevant information (location, nature of emergency, medical data, live updates).
- Resource registries: Databases of AED locations, first aid kits, and safe sites. Some public systems already maintain AED registries linked to responder apps.
- Privacy and security controls: Protections against stalking, malicious use, and data leakage, such as delayed location disclosure, anonymity options, and encryption. The use of wearables raises questions about persistent identifiers and tracking.
Real-world implementations typically use smartphones rather than NFC wearables, but the NFC ring is a recurring design motif because it suggests a "civic interface": a physical token that makes help-seeking socially legible and technically simple.
Use Cases
Medical Emergencies
The most common contemporary use case is mobilizing nearby help for cardiac arrest and other time-critical medical events. Systems that dispatch volunteer responders through smartphone apps aim to increase early CPR and AED use before EMS arrival.
In Australia, programs such as GoodSAM have been used by ambulance services to alert nearby volunteers to suspected cardiac arrests, illustrating the proximity-based model of response. Studies continue to evaluate these systems' impact on survival and process measures (e.g., time to CPR, time to defibrillation).[3]
Personal Safety and Public Incidents
A civic proximity response system may also be applied to personal safety incidents—assault, stalking, falls, or situations where a person feels unsafe but cannot safely call. In such designs, the system may notify nearby designated responders (venue staff, security, trained community members) while also creating a record that can assist later investigation.
Because false alarms and malicious triggering can impose social and policing costs, safety-oriented systems often emphasize graded escalation, silent alerts, and verification mechanisms.
Family and Domestic Violence
Domestic and family violence contexts are frequently discussed in relation to rapid alerting, monitoring, and protective interventions. In practice, two distinct approaches are often grouped together:
- Victim-initiated alerts (panic alarms, duress buttons, emergency phone features), intended to speed police response or activate a support network.
- Perpetrator-focused measures (e.g., electronic monitoring), intended to deter breaches and support enforcement of restraining orders.
Evidence is mixed and context-dependent. A 2022 review comparing panic alarm systems for high-risk domestic abuse noted variability in design and outcomes and discussed the limited published evidence base, including at least one study reporting potential unintended effects in a specific setting.[4]
In Australia, evaluations of electronic monitoring programs for domestic violence offenders have reported associations with reduced reoffending for monitored cohorts compared with similar non-monitored cohorts, while also noting methodological limitations typical of non-randomized designs.[5]
Evidence and Evaluation

Community First Responder Dispatch
Research into smartphone-dispatched volunteer responders has expanded, especially in cardiac arrest response. A 2025 report in the Medical Journal of Australia discussed associations between smartphone-activated volunteer responders arriving before EMS and improved survival to discharge after out-of-hospital cardiac arrest in the studied setting.[6]
Common evaluation metrics include:
- time from collapse to CPR
- time to first defibrillation
- rates of bystander CPR and AED use
- survival to hospital discharge and neurological outcomes
- responder arrival times relative to EMS
- false alarm rates and operational workload
Safety and Domestic Violence Technologies
Evidence for panic alarms and duress devices in domestic abuse contexts is less standardized, with heterogeneity in device design, policing protocols, and victim circumstances. Reviews emphasize that panic alarms often function as part of a broader safeguarding package (risk assessment, police prioritization, support services), and outcomes may depend heavily on implementation details.
Evaluations of offender electronic monitoring in domestic violence contexts, including Australian programs, suggest potential reductions in recidivism or custody outcomes, but causal interpretation remains difficult without randomized assignment and with possible unobserved differences between monitored and unmonitored groups.
Limitations, Risks, and Criticism
Civic proximity response systems face several recurring critiques:
- Safety of responders: Mobilizing untrained citizens into unpredictable scenes can increase risk of harm, especially in violent incidents or situations involving weapons, intoxication, or severe mental distress. Systems may need strong triage, role-limiting, and "observe and report" options.
- False alarms and misuse: Low-friction triggers can be abused, creating alert fatigue or unnecessary police attendance. Verification measures can reduce misuse but may increase friction for genuine emergencies.
- Equity and coverage: Proximity response depends on smartphone access, density of volunteers, and public trust. Rural areas, disadvantaged communities, and marginalized groups may receive uneven benefits.
- Privacy and surveillance: Location-based alerting and wearables raise issues of tracking, data retention, and secondary uses of data. Victims of stalking may be at particular risk if systems leak location or identity.
- Over-reliance on citizen labor: Critics argue that shifting responsibility to citizens can become a rationale for underfunding professional emergency services. Proponents counter that the goal is not substitution but the narrowing of the gap between incident onset and professional arrival.
- Normative coercion: Some argue that formalizing civic obligation—especially through criminal penalties—can produce coercive expectations, disproportionately affecting people who are afraid, disabled, or uncertain.
Implementation Considerations
Designers and policymakers proposing civic proximity response systems often emphasize:
- Clear role design: Most bystanders should not be expected to "intervene" directly; they can be empowered to signal, support, and stabilize.
- Training and micro-instructions: Short, context-specific guidance (e.g., CPR prompts, safe positioning, de-escalation tips) can reduce hesitation and harm.
- Integration with existing infrastructure: Linking to emergency call centers, AED registries, and venue safety plans is usually more effective than standalone apps.
- Governance and accountability: Transparent policies on data retention, auditing, and oversight can help maintain trust, especially where police involvement is possible.
- Abuse-resistance: Mechanisms such as rate-limiting, reputation systems, responder verification, and "silent activation" options may be required.
Conceptual Variants
Related models include:
- Personal emergency response systems (PERS), including medical alert pendants used primarily by older adults.
- Mass notification systems used by campuses and municipalities, typically for hazards rather than individualized emergencies.
- Mutual aid networks, which coordinate community support outside formal emergency services, often during disasters.
- Mesh-network emergency tools, designed to function when cellular networks are unavailable (e.g., disaster scenarios), sometimes combined with local radio or satellite links.
Additional References (Civic Proximity Response)
Key sources used in discussion of duty-to-assist law and technology-mediated volunteer dispatch include official French public guidance on failure to assist, the French Penal Code provision commonly cited for non-assistance à personne en danger, peer-reviewed clinical and registry studies on smartphone-activated volunteer responders, and evaluations of domestic violence electronic monitoring programs and panic alarm systems.
- ↑ Effect of Smartphone Dispatch of Volunteer Responders on Cardiac Arrest Outcomes. PMC, 2022.
- ↑ Article 223-6 - Code pénal. Legifrance.
- ↑ The effect of the GoodSAM volunteer first-responder app on cardiac arrest outcomes. OUP Academic.
- ↑ Comparing panic alarm systems for high-risk domestic abuse. PMC.
- ↑ An evaluation of the NSW Domestic Violence Electronic Monitoring program. BOCSAR.
- ↑ Smartphone-activated volunteer responders and survival to discharge after out-of-hospital cardiac arrest. MJA, 2025.